Abscess
Oral micro-organisms can reach the periapical tissues (structures adjacent to the tip of root) via the root canal system or via the periodontal ligament (connective tissue fibres that attach a tooth to its position in the bone). If the bacteria are sufficiently virulent and/or the host defences compromised then the infection may give rise to a dentoalveolar abscess (a dental abscess; most commonly a periapical abscess or a periodontal abscess).
The face has a layer of superficial connective tissue, mainly collagen, beneath the skin, the facial fascia. The complex attachment of the facial fascia determines how these infections spread.
An abscess may remain localised and drain via a small intraoral sinus (a ‘gum boil’, see Figure 1) or may spread giving rise to a severe cellulitis involving multiple tissue spaces (a cervicofacial abscess, see Figure 2).
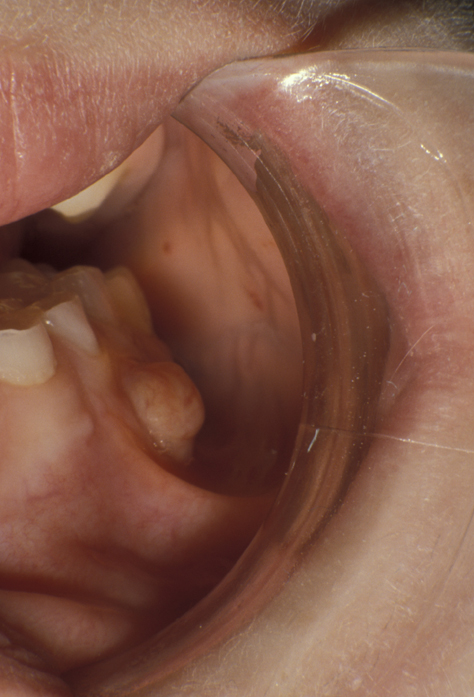
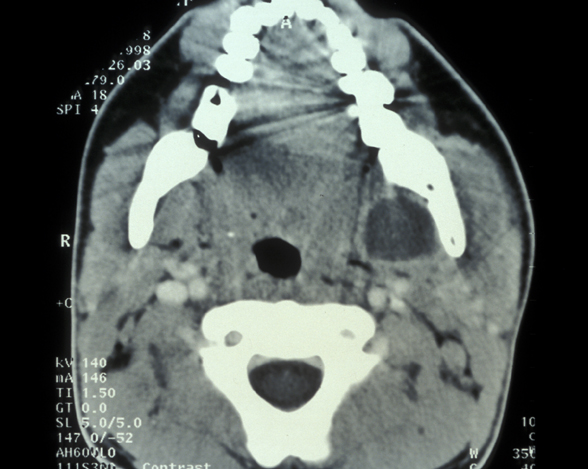
A variety of organisms are involved in these infections. Alpha-haemolytic streptococci, non-haemolytic streptococci, Gram-negative cocci, actinomyces species, actinobacillus actinomyetemcomitans and Gram-negative anaerobic rods are all observed. There is an increasing recognition of the role of anaerobic bacteria, especially streptococci in these infections.
The specific signs and symptoms will depend on which tissue spaces are involved. The symptoms may include: pain, swelling, discharge, tenderness to percussion of involved teeth, trismus (difficulty opening the mouth) and dysphagia (difficulty swallowing). Trismus or dysphagia, particularly for fluids (it may be even impossible to swallow one’s own saliva) are warning signs that the airway may be at risk. Systemic upset is variable, but may manifest as pyrexia, tachycardia and hypotension (fever, fast heart beat and low blood pressure). Infections of the anterior maxilla (the front of the upper jaw) may rarely give rise to cavernous sinus thrombosis, a condition which still has a mortality of 30% despite antibiotic therapy. The signs of a blood clot forming in the hollow spaces behind the eye sockets (a cavernous sinus thrombosis) include proptosis (bulging of the eye), chemosis (swelling of the inside of the eyelids), ophthalmoplegia (impaired eye movements) and marked systemic upset.