Bleomycin
The bleomycin group of closely related organic compounds are natural products, produced by a bacterium, streptomyces verticillus, but have also been synthesized in the laboratory (Figure 1).
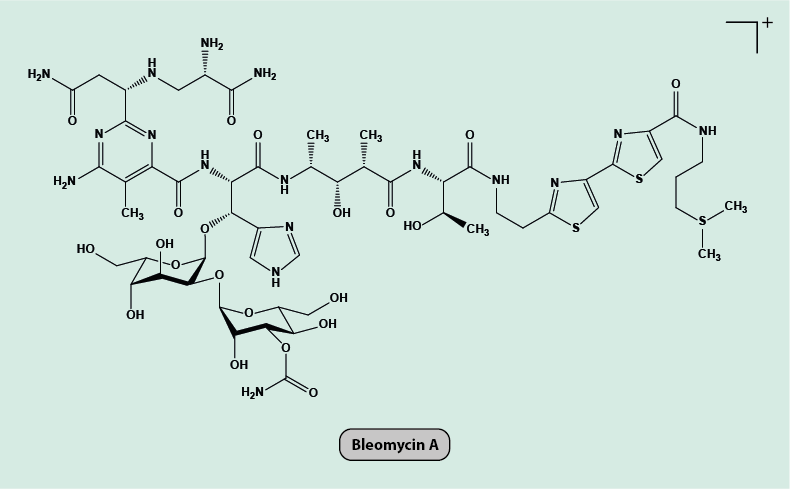
Bleomycin was originally intended as an antibacterial agent, in line with the common traits of many bacterial strands in producing naturally occurring antibacterial agents as a defence of their own bacterial communities against competing bacterial strands. The considerable toxicity of bleomycin has prevented its application as an antibacterial agent. Systemic use of bleomycin is associated with a significant burden of pulmonary toxicity, leading to pulmonary fibrosis (scarring) and reduced lung function.
Instead, bleomycin has found some role in the chemotherapy of some malignancies, in particular Hodgkin’s lymphoma where it is used as a component in multi-agent chemotherapies, combined with several other cytotoxic agents. In the 1980s and 1990s bleomycin was also used in combination chemotherapies of head and neck malignancies, mostly in combination with cisplatin and in the palliation of advanced disease, with limited success.
Another, non-systemic, application of bleomycin is in the treatment of vascular malformations. For non-systemic use of bleomycin, such as intralesional injection as a sclerosing agent in the treatment of vascular malformations, no pulmonary toxicity has been observed in the short term but further investigations of long-term effects are necessary. Bleomycin has been found to be a safe and effective sclerosing agent for the treatment of a range of vascular malformations in the head and neck region, with fewer local adverse effects reported than for other sclerosing agents. More recently, combined treatment schemes comprising of bleomycin sclerotherapy and Nd:YAG laser treatment for venous malformations in the head and neck region also have been advocated as safe and effective treatment modalities. About 25 years ago, bleomycin was briefly used topically on oral premalignant lesions but never became an established treatment modality.
The mechanism(s) by which bleomycin is cytotoxic have been researched for many years. There are a number of hypotheses about these mechanisms of action. It is generally agreed that bleomycin interferes with DNA, causing DNA strands to break. One line of thought is that a number of different chemical reactions in a cascade of events lead to this effect. This view is based on laboratory observations where it was demonstrated that the presence of iron ions and oxygen is necessary for this cytotoxic effect to occur. The damage to DNA is then ultimately caused by the formation of reactive oxygen species (radicals; which is very similar to the main cytotoxic effects of high-energy radiation in radiotherapy) at the end of this cascade of chemical reactions. Another line of investigations postulates a direct interaction of bleomycin with DNA by binding to specific sites of DNA. In this way, the cleavage of DNA molecules is enabled by a direct chemical reaction mechanism between DNA and bleomycin. In addition, it has been shown that bleomycin enhances the degradation of yet another fundamental cellular component, RNA. This represents another route to causing cell damage as RNA is essential for the normal function of all cellular metabolic processes.