Oral mucosal lesions
Contents
Our discussion of treatment options for oral mucosal lesions mirrors the organisation of the corresponding section on the diagnosis of oral mucosal lesions.
Oral mucosal lesions related to infections
Oral infections are common and represent a diverse range of conditions, including infections specifically affecting the mucosa. Accordingly, bacterial, fungal and viral oral infections and their treatment are discussed in several sections of the website:
Recurrent aphthous stomatitis (mouth ulcers)
Recurrent mouth ulcers (Figure 1), be they minor or major lesions, have one aspect in common: there is considerable overlap between the detective work of arriving at a diagnosis and identifying underlying causes, and the resulting treatment paths.
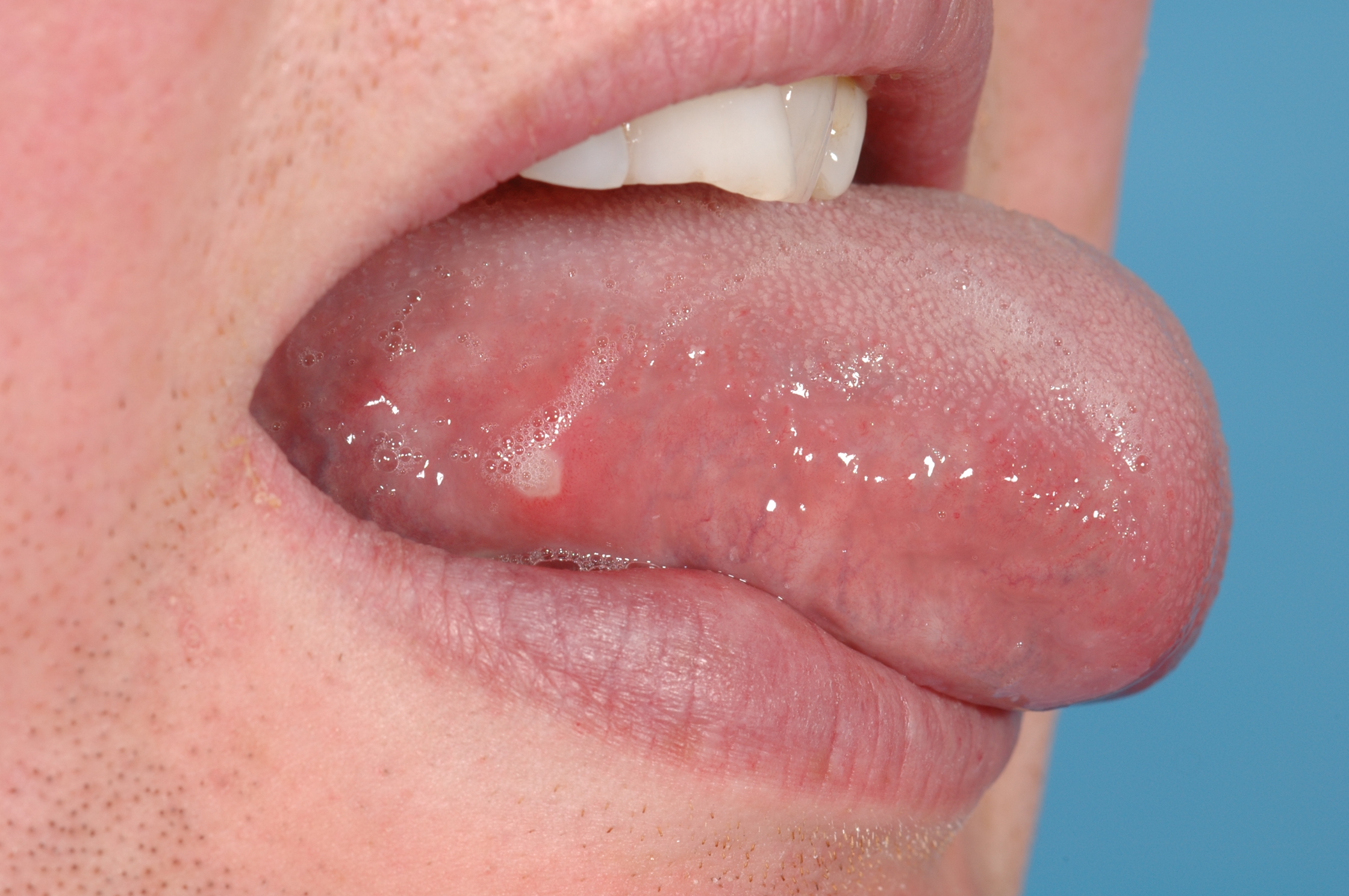
The long-term view of treatment decisions for minor aphthous ulcers needs to be backed by identification and/or exclusion of underlying condition(s), mostly relying on detailed medical history and a range of blood tests.
Where local trauma is the cause, such as an ill-fitting denture or a sharp edge of a tooth, dealing with this mechanical irritant removes the cause for recurrent mouth ulcers.
Where an underlying condition and relation with a disease (see below) are identified as the cause, successful treatment of these conditions (after referral to the appropriate specialty) will resolve recurrent mouth ulcer problems too. Where some deficiency such as a low level of iron or vitamin B12 is identified as the cause, supplementing these low levels is necessary, in addition to further investigations about the underlying cause(s) for the deficiency.
Where aphthous ulcers occur because of a reaction to an irritant or allergen, avoiding known irritants/allergens is the best approach. The list of potential irritants/allergens is long, but there are some common causes. Examples are intolerance to gluten, to sodium lauryl sulfate (a common detergent and foaming agent in toothpastes), to some food ingredients, or to smoking.
A number of drugs, including analgesics, in particular nonsteroidal anti-inflammatory drugs (NSAIDs), a range of antihypertensive drugs (the vasodilatory drug nicorandil is a well-recognised example) and other agents for the treatment of cardiovascular conditions and some bisphosphonates, are known to cause stomatitis problems. Ideally, a drug causing recurrent mouth ulcers should be avoided or, where that is not an option, an alternative drug should be tried. These choices may be a delicate balancing act between wanted and adverse effects of a drug. There may be situations where there are no alternative drugs, or where it would not be reasonable to stop taking a particular drug.
The short-term view of the treatment / management of acute minor aphthous ulcers needs to focus on the prevention of superinfections and pain relief. This typically includes the use of chlorhexidine mouthwash and general attention to optimal oral hygiene, a range of analgesics (including topical applications, such as benzydamine mouthwash) and/or topical steroid applications such as hydrocortisone gel. The typical appearance of a healing aphthous mouth ulcer is depicted in Figure 2.
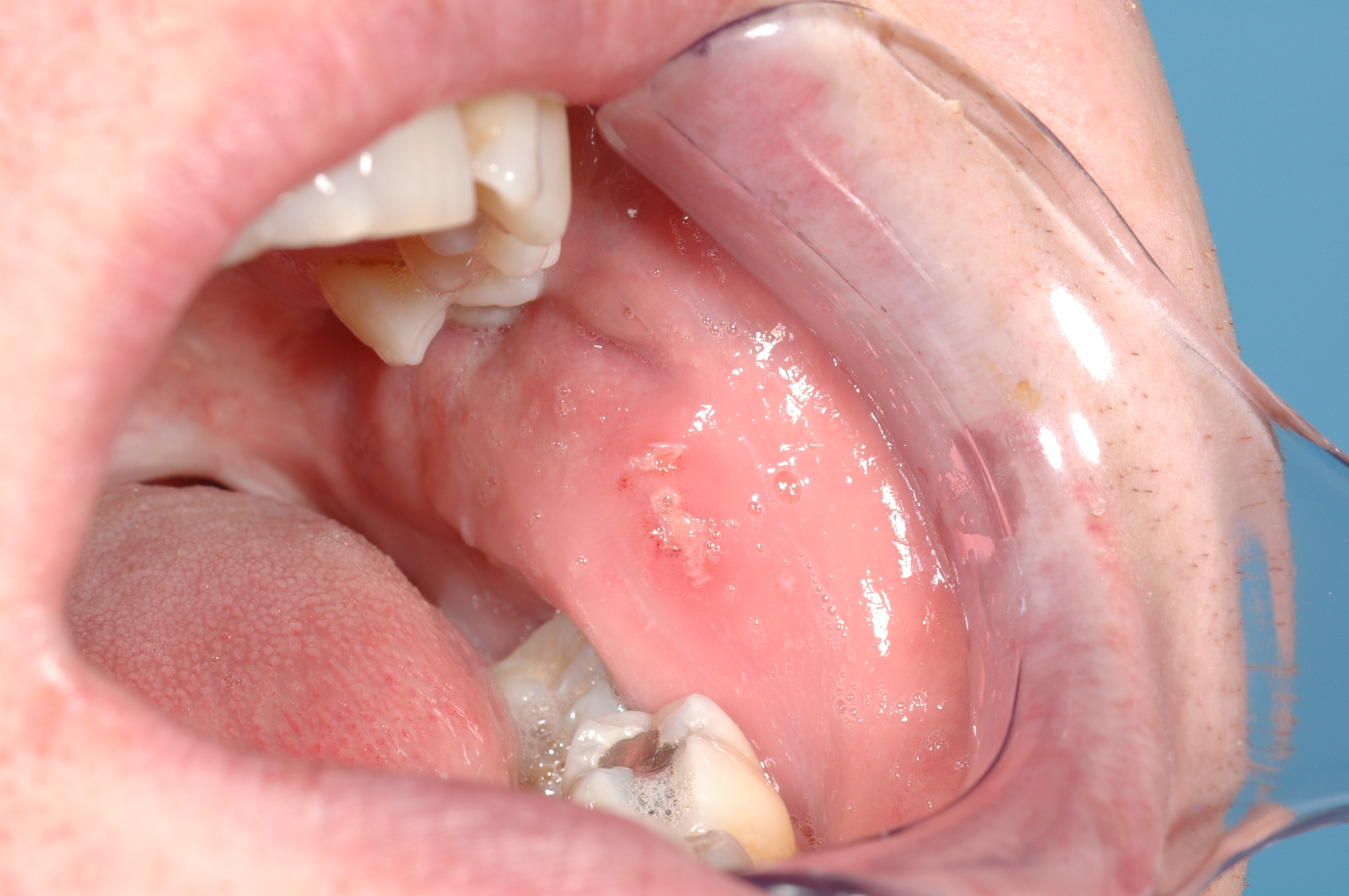
Treatment schemes for major aphthous ulcers and herpetiform ulcers are essentially the same as for minor aphthous ulcers, but are more likely to require systemic steroids and these lesions have a higher probability for being a symptom of a gastrointestinal disorder. Treatment of oral mucosal lesions as one of several symptoms of Behçet’s disease may require potent anti-inflammatory agents such as anti-TNF agents (a monoclonal antibody), in joint treatment approaches with rheumatology and/or ophthalmology.
Mucositis
Oral mucositis is a severe and painful adverse effect that occurs in nearly all people receiving treatment with radio- and/or chemotherapy for head and neck cancer. Severe oral mucositis also is a common adverse effect of chemotherapy treatment for blood malignancies and may occur after bone marrow transplants.
For the moment, there is no convincing strategy or treatment plan to prevent this debilitating condition altogether. However, some strategies may help to reduce severity and/or duration of oral mucositis. Treatment of oral mucositis in general is geared toward optimal management of symptoms.
There is circumstantial evidence that cryotherapy in the form of ice chips held in the mouth, may have some limited benefit in preventing oral mucositis from chemotherapy. It is thought that the low temperature leads to vasoconstriction and thus reduces the amount of cytotoxic drug(s) delivered to the oral mucosal tissue.
The use of keratinocyte growth factor, palifermin (which stimulates tissue growth, including the oral mucosa) is controversial for a number of reasons, including its potential for promoting the growth of non-haematological malignancies and interference with some chemotherapy treatment schemes. Amistofine is a cell-protective agent. It is a prodrug which relies on a specific hydrolysis mechanism for activation that is likely not to be active in malignant cell lines, so it is considered safe as it is not likely to protect malignant cells from high-energy radiation effects. Studies have shown that amistofine can reduce xerostomia (dry mouth) problems during head & neck radiotherapy treatment cycles, but there is no convincing evidence of long-term advantages. Amistofine has also been suggested as a cell-protective agent for the prevention of oral mucositis but there is little convincing evidence in support of this use.
Some modest evidence exists for a number of interventions aiming at reducing severity and duration of oral mucositis.
Sucralfate is a complex of sucrose octasulfate with aluminium hydroxide. It dissociates in the acidic stomach environment, where it subsequently forms a protective film on the stomach lining; sulfacrate is used in the treatment of stomach ulcers. In this form, sucralfate is not effective in the management of oral mucositis because the oral cavity is not an acidic environment. However, polymeric viscous paste-like preparations of sucralfate adhere to the oral mucosa and to oral ulcers, forming a protective layer and thus supporting healing. Making best use of the combined various available options for best possible relief from symptoms, for example could be use of benzydamine mouthwash (for analgesia), followed by chlorhexidine mouth rinse (for antisepsis) and completed by the application of a sealant-gel preparation for prolonged protection and pain relief.
Low-intensity laser-therapy, LILT is also thought to support and accelerate the healing process, by stimulating tissue regeneration. The approach uses low-intensity coherent laser light in the visible red to infrared region of the spectrum of electromagnetic radiation. Although the working mechanisms are not well understood, it is thought that this form of ‘phototherapy’ has some stimulating effects on cell proliferation as well as some anti-inflammatory effects, and thus can support healing.
For a fair number of further suggested interventions aiming to reduce symptoms of oral mucositis, there is only weak, or no evidence of significant beneficial effects. These suggestions include topical use of honey or royal jelly (the hypothesis for its working mechanism is its high sugar content which acts as a drying agent on the oral mucosa and any ulcers; the high sugar content makes honey a double-edged sword in that it will also promote dental decay), aloe vera preparations, antibacterial lozenges, lactobacillus brevis lozenges (aiming to strengthen the microbiome in the oral cavity, similar to the assumed benefits of probiotics on the gut flora), zinc supplements in the form of zinc sulfate, ZnSO4 mouthwash (Zn2+ ions are an essential mineral for the proliferation of epithelial cell lines). There are also numerous ‘alternative medicine’ suggestions for the management of oral mucositis, but there is no evidence that any of these have any benefits.
The core focus of current therapy and management of oral mucositis remains the provision of adequate pain control, the best possible maintenance of the oral mucosal condition, and prevention and/or treatment of any infections. Severe oral mucositis may make oral food intake temporarily impossible and necessitate a period of non-oral feeding via a feeding tube. Extreme oral mucositis can be a treatment-limiting adverse effect of ongoing oncological treatment. When swallowing is difficult or impossible, changing the delivery method of all medications from oral intake to other delivery methods is necessary.
Best possible maintenance of oral hygiene is an essential contribution to limit oral mucositis, both keeping an appropriate daily routine at home and regular support by a professional oral hygienist. Use of bland saline mouth rinses throughout the day can provide symptom relief and help maintain a healthy oral environment. Alcohol-containing mouth rinses are not recommended because of the drying effect of alcohol on the mucosa (they are also painful).
Where infections occur, the usual steps for the treatment of oral infections, predominantly by antimicrobial agents are taken.
Topical delivery of analgesia is the desirable delivery method if adequate pain control can be achieved in this way and safe swallowing has been confirmed (so that there is no danger of aspiration of any of the topical agents for oral use) – topical delivery reduces the overall load of systemic drugs on the body. Topical analgesic agents include viscous lidocaine-containing pastes, benzydamine mouthwashes, a variety of steroid anti-inflammatory preparations, or morphine mouthwash. If topical pain control is impossible or fails, systemic analgesia is necessary, often delivered intravenously or via transdermal patches. As with most pain management it has been shown that in these circumstances scheduled administration of analgesics is more effective than administration as needed.
Vesiculo-bullous lesions (blisters)
When infections, in particular viral infections are the cause, the condition will either be self-limiting or any active treatment will address the infecting microbes and management of discomfort and pain.
The other main causes for oral vesiculo-bullous lesions are a range of different autoimmune disorders, in need of different treatment schemes. Some autoimmune conditions require urgent and intensive treatment, often including systemic immunosuppression. There are two main scenarios where and when treatment is provided. The first point of contact may be an oral and maxillofacial surgery clinic, if oral symptoms are the only or predominantly problems. Otherwise, there may have been a referral from another specialty such as rheumatology, in order to deal with oral symptoms of a systemic disease.
In either case, and in line with the treatment of most autoimmune conditions, treatment modalities are usually a joint effort between different disciplines. The role of oral and maxillofacial surgery is to maintain and monitor oral health and integrity of the oral mucosa as far as possible, in addition to management of discomfort and pain as the burden of oral symptoms of these conditions can be considerable. Maxillofacial surgery oversight and advice is helpful in trying to prevent infections and/or formation of oral ulcers. Blisters of the oral mucosa are easily ruptured just by the normal function of mouth and jaws, causing painful oral ulcers and infections.
The general treatment approaches for serious autoimmune conditions such as pemphigoid or pemphigus vulgaris typically include immunosuppression topically (for example, application of steroids) and/or systemically. Not all of these conditions can be treated successfully with steroids, but may require medication schemes with monoclonal antibodies and similar targeted approaches for the management of different autoimmune conditions. Some of these conditions may be difficult to treat. Many different medication protocols with additional drugs have been suggested (and continue to be suggested) but there is little clear evidence that any of these combination-medication schemes achieve better result than steroids alone. However, there seems to be a shift of practice to consider monoclonal antibody therapies as the first-line treatment for some of these autoimmune conditions, replacing steroids as the first-line choice of medication in some cases.
Another condition, angina bullosa haemorrhagica, is not an autoimmune disorder but its underlying causes remain somewhat mysterious. Accordingly, treatment is entirely symptomatic, in keeping with an odd but harmless condition that we essentially do not understand.
Persistent patches and lesions
Persistent white (leukoplakia), red (erythroplakia) and speckled (erythroleukoplakia) patches, submucous fibrosis (scar tissue formation beneath the mucosa) and some rare variants of lichen planus (see below) all belong to a group of oral lesions that are associated with variable degrees of abnormal cell growth (dysplasia) and a possibility for malignant transformation of the lesion. These premalignant lesions all require long-term monitoring and repeated decisions about surgical or other interventions.
Oral lichen planus, the mucosal variant of a common skin condition, is a chronic condition and requires long-term management. Oral lichen planus can be asymptomatic or a rather debilitating condition with a severe symptom burden, especially erosive and ulcerative forms of the condition (Figure 3). The term oral lichen planus covers a range of similar conditions. The potential of oral lichen planus for malignant transformation remains a matter of debate. It has been estimated that there may be a 1 to 3 % risk for malignant transformation.
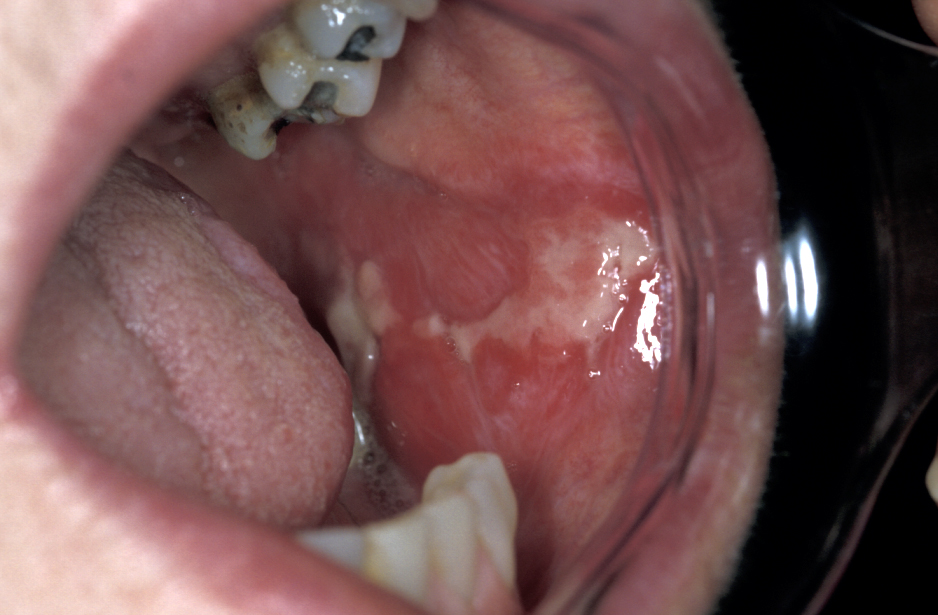
The chronic nature of the condition, combined with diagnostic difficulties, a potentially significant morbidity (in particular pain) and an insufficient understanding of the cause(s) all contribute to the need for patience on behalf of all involved. This situation also accounts for the fact that there is no widely agreed therapeutic approach for the management of this group of conditions.
The topical application of a number of different steroids remains the first-line medication scheme. This could be in the form of sublesional injections, but some patches drenched with a slow-release form of clobetasol (a corticosteroid) are also being tested. Failure of the lesions to resolve under topical treatment with steroids is not uncommon. In such cases, topical application of a different type of agent, a calcineurin inhibitor (immunomodulating agents that reduce inflammation) such as tacrolimus or pimecrolimus may offer an alternative.
For persistent cases that do not resolve under topical treatment schemes, systemic steroid therapy may be necessary. Other treatment schemes favour the use of low-intensity laser therapy, LILT rather than pharmacological drugs. Some studies have demonstrated that LILT helps with pain management, can reduce the clinical signs of oral lichen plans, is similarly effective as more established drug treatments and avoids the adverse effects of, for example, systemic steroids. It remains to be seen if these initial findings about LILT can be confirmed in larger systematic and rigorous studies. Surgical excision combined with soft tissue grafts for repairing the defect has been suggested for the treatment of isolated but persistent oral lichen planus lesions and may offer an alternative treatment modality in some limited circumstances.
Similar to most of the other oral mucosal lesions discussed here, oral lichen planus may be triggered by some medications (in particular non-steroidal anti-inflammatory drugs (NSAIDs) and beta-blockers (agents to reduce high blood pressure have been associated with oral lichen planus) or by some local irritant(s) such as amalgam dental fillings. If such a cause can be identified, avoiding the cause where possible is the obvious way forward. The various beliefs of clinicians without any real evidence base can create conflict in this area. Some clinicians advocate removal of all amalgam fillings on the basis of their belief (justified by a very limited evidence base) that amalgam can cause severe oral lichen planus in some people. Others completely refute this (again justified by a very limited evidence base). One, relatively logical way forward would be to accept amalgam may be a cause if a large metal filling is associated with a prominent localised patch of oral lichen planus and deal with that.
Frictional keratosis (caused by some minor local trauma) and smoker’s keratosis (caused by irritants in tobaccos smoke) are dealt with by simply eliminating the respective irritant.
Oral cancer
The majority of oral mucosal lesions are benign. If, however, a lesion has been identified as malignant, the whole range of treatment schemes for oral malignancies will need to be considered and any decisions about the individually best possible treatment option(s) depend on type and extent of the malignancy as well as on personal situation and preferences.
All these aspects of diagnosis and treatments for oral cancer are discussed in detail on several dedicated pages, including
- surgical treatment options;
- reconstructive surgery;
- restorative dentistry, including specific kinds of prostheses;
- radiotherapy;
- chemotherapy;
- new developments, such as immunotherapies;
- a whole range of relevant help and self-help themes.
Oral mucosal lesions related to other diseases
With many non-oral diseases having oral manifestations, the role of oral and maxillofacial surgery in the treatment of such conditions is collaborative (with those specialties responsible for treating the underlying condition(s)) and supportive in monitoring and managing oral signs and symptoms. Non-oral disease with oral manifestations mainly include
- gastrointestinal disorders (unsurprising in that the mouth is a part of the gastrointestinal tract);
- skin disease which may equally or predominantly affect mucosa, including oral mucosa;
- haematological disorders.